If you are like us, you taken many vestibular therapy courses without being taught how to treat BPPV affecting the anterior canal. Granted, BPPV affecting the anterior canal is rare. If you, however, see a lot of patients with dizziness you will likely see this form of BPPV at some time. When that does occur what are your options?
- Search Dr. Google and hope for the best.
- Ask a colleague.
- Figure it out using an anatomical model (if you have one).
- Hope it will resolve spontaneously.
- Other.
Given such, let’s review a treatment option that we have found simple and effective called the Deep Head Hand Maneuver. Before we review the technique let’s review some background information.
How often does BPPV affect the anterior canal?
As we have all been told BPPV affecting the anterior canal is rare. According the 2017 Clinical Practice Guidelines, BPPV affecting the anterior canal accounts for up to 3% of those who develop BPPV. 85-95% of the time it involves one of the posterior canals. 5-15% of the time it involves one of the lateral canals. Given the prevalence of BPPV affecting the posterior and lateral canals most of the training in the field of vestibular therapy has focused on BPPV affecting these two canals, with the anterior canal often being neglected.
How can you tell if the anterior canal is affected?
BPPV affecting any canal will elicit nystagmus with positional testing. Positional testing includes, but is not limited to the Dix-Hallpike test, Loaded Dix-Hallpike test, and the Roll test.
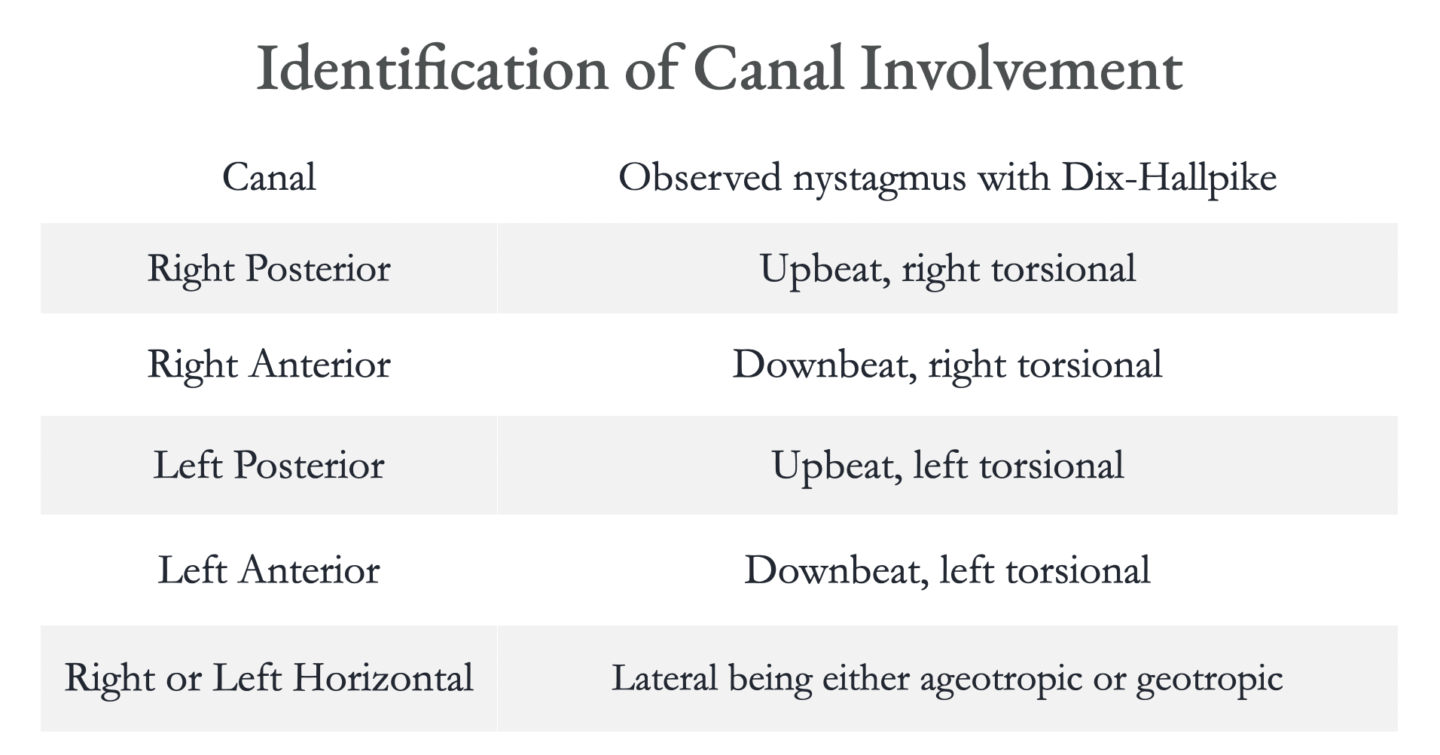
The direction of the nystagmus indicates the canal involved:
The above chart indicates the canal involvement with Dix-Hallpike testing, but these results can be elicited with other positional tests as well. So, anterior canal involvement will be evident with downbeat, torsional nystagmus with positional testing. Unlike the posterior canal it may be positive for downbeat nystagmus that has the same torsional component when tested to either side.
With the downbeat nystagmus how can I be confident that the this is not a central vestibular problem?
In the rare case that there is BPPV affecting the anterior canal, the torsional component may not be easy to see. Having the patient look to one side with their eyes may increase the torsional component. Here is a video that dives deeper into this tip. If looking to the side does not increase the torsional component here are some other tips to help determine if the nystagmus is due to BPPV affecting the anterior canal or due to a central vestibular disorder:
- With BPPV look for an increase in nystagmus when visual fixation is absent (will need infrared goggles). There will be no change in the intensity of the nystagmus with a central vestibular disorder with and without visual fixation.
- With BPPV affecting the anterior canal there may be a reversal of the nystagmus when the patient is sat up which will not occur with a central vestibular disorder.
- With a central vestibular disorder there will be no delay with the nystagmus and symptoms, which will also be present with cupulolithiasis of the anterior canal. Note that cupulolithiasis is a less common form of an already rare form of BPPV.
- With BPPV, unless it is cupuloithiasis [remember, less common form of an already rare form of BPPV] the nystagmus should last less than a minute.
- You can try a canalith repositioning technique (as outlined below) and if it is BPPV it should resolved rapidly with treatment.
- With a central vestibular disorder it will not fatigue with repeat positional testing as it will with BPPV.
If in doubt assume it is a central vestibular condition and manage accordingly.
Head position maneuvers to treat anterior canal BPPV
Remember that anterior canal BPPV is rare and that canalithiasis is more common that cupulolithiasis. So, to treat canalithiasis affecting the anterior canal there are several options that include:
- The Deep Head Hang Maneuver.
- The modified Epley (with some tweaks to the traditional modified Epley).
- The Kim Maneuver.
- Other.
Our “Go To” technique at North 49 is the Deep Head Hand Maneuver. It is super simple and effective. It is also forgiving in that it does not matter if you are treating the right or left anterior canal, the treatment is the same.
Deep Head Hang Maneuver how to perform
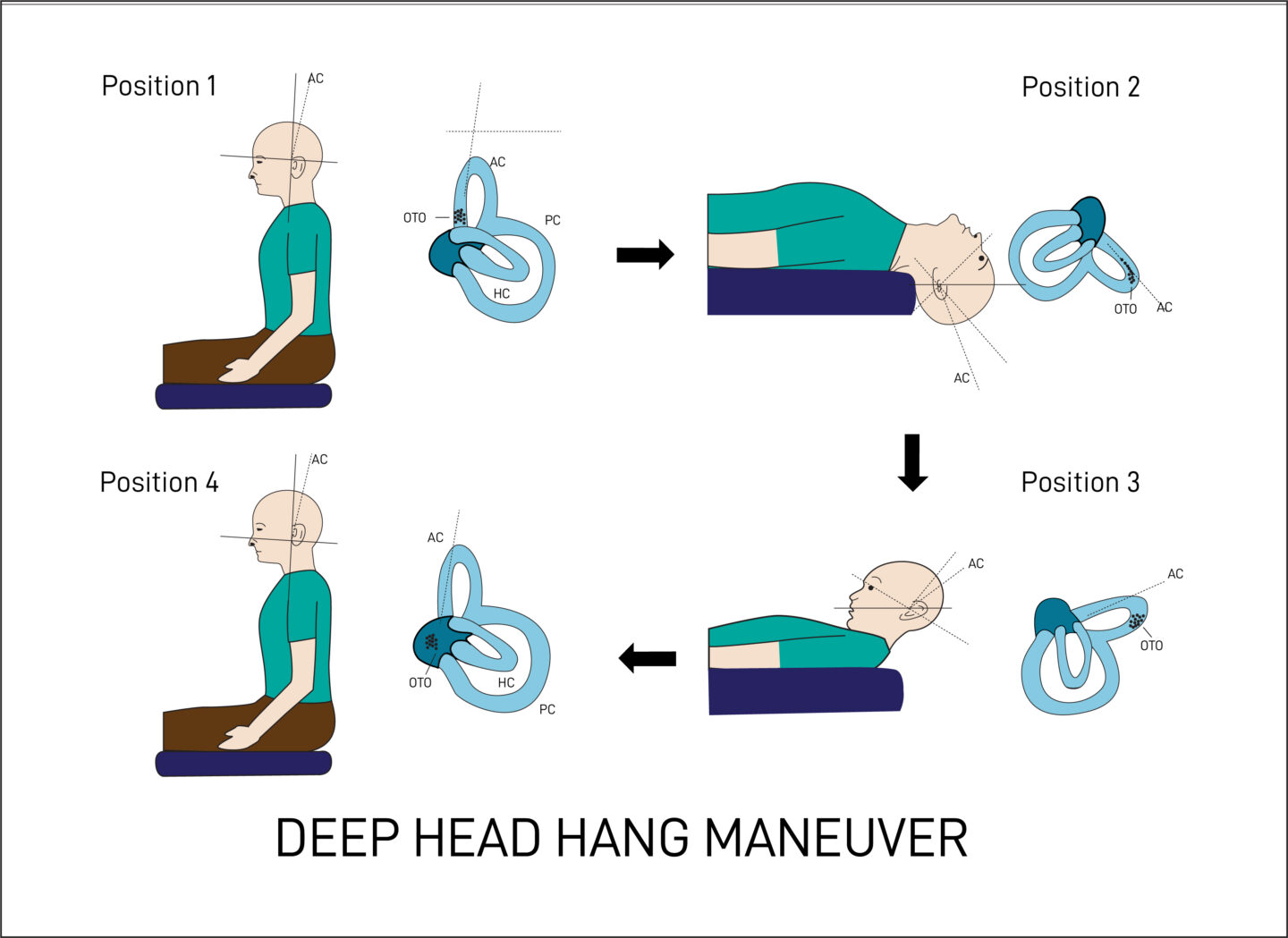
As per Yacovino (2009) the maneuver consists of 4 steps:
- In sitting with neck in neutral.
- Lay back supine with at least 30o of neck extension. Hold this position until the nystagmus and dizziness stop, then an additional 30 seconds.
- While supine quickly move the chin to the chest and hold this position until the nystagmus and dizziness stop, then an additional 30 seconds.
- Sit the patient up and put the neck into a neutral alignment and hold this position until the nystagmus and dizziness stop, then an additional 30 seconds.
To see an instructional video of how to perform the Deep Head Hang Maneuver click HERE.
How the Deep Head Hand Maneuver works
If you are like us, we like to see things visually to understand what is happening when this maneuver is performed. Given such we have filmed this brief video that uses a fluid filled 3D anatomical model to demonstrate what is thought to happen during this maneuver.
Conclusions
BPPV is the most common cause of dizziness across the lifespan, with the posterior canal being affected the most often. On the rare occasion it can, however, involve the anterior canal and clinicians should be aware of how to address this, should it occur.
At North 49 we have found the Deep Head Hang Maneuver a simple and effective option to treat anterior canal BPPV when it does occur.
To learn about other options for treating BPPV affecting the anterior canal they can be found in A Field Guide to BPPV, which is a 6.5 hour online course we developed and is accredited for CE hours in over 40 states. North 49 also offers weekend and hybrid courses in the area of BPPV and other vestibular related topics.
If you have any questions regarding this post, please feel free to contact us at contactus@north49therapy.ca.