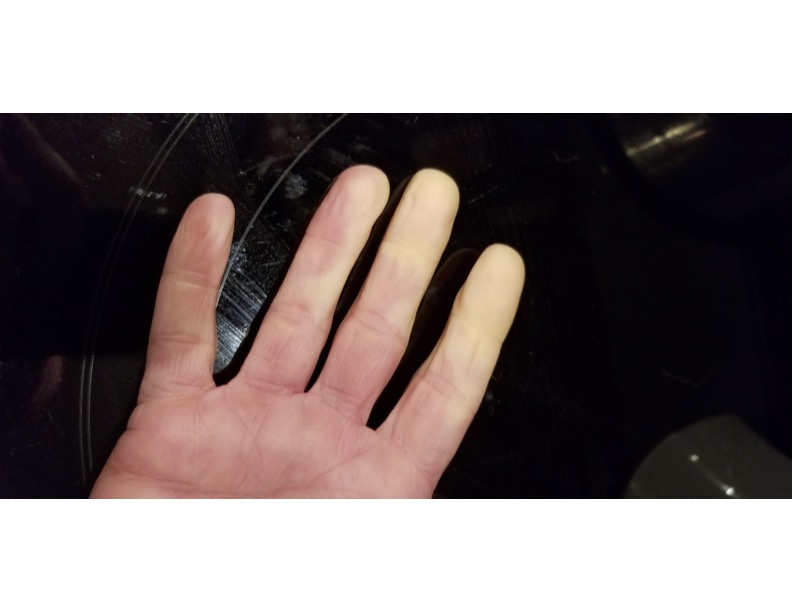
Fingers and toes that are always cold could be a sign of Raynaud’s. Raynaud’s affects some areas of your body, most often your fingers, and less commonly your toes, nose, lips or ears, causing them to change color and feel numb and cold in response to cold temperatures or stress. It can be painful or you may have a “pins and needles” sensation. It is due to the small blood vessels in the fingers “spasming,” reducing blood flow to the fingertips.
Here is a link to an interesting video about Raynaud’s
Why does Raynaud’s occur?
We don’t completely understand the cause of Raynaud’s, but blood vessels in the hands and feet appear to overreact to cold temperatures or stress. The arteries to your fingers and toes become narrow and limit blood supply when exposed to cold or stress.
Exposure to cold temperatures, such as putting your hands in cold water, taking something from a freezer or being in cold air, is the most likely trigger for an episode of Raynaud’s. Emotional stress can also be a trigger for some people.
There are two main types of Raynaud’s:
- Primary Raynaud’s is also called Raynaud’s disease and isn’t associated with a medical condition. It can be so mild that some people with primary Raynaud’s don’t seek treatment. It can resolve on its own. This is the more common type of Raynaud’s.
- Secondary Raynaud’s is called Raynaud’s phenomenon and is caused by an underlying problem. Although secondary Raynaud’s is less common, it tends to be more serious than primary Raynaud’s.
Causes of secondary Raynaud’s include:
- Connective tissue diseases. Most people who have scleroderma, a rare disease that leads to hardening and scarring of the skin, have Raynaud’s. Other diseases which may be associated with Raynaud’s include lupus, rheumatoid arthritis and Sjogren’s syndrome.
Some information about scleroderma.
- Diseases of the arteries, including a buildup of plaques in blood vessels which feed the heart, inflammation of blood vessels of the hands and feet or a type of high blood pressure which affects the arteries in the lungs.
- Carpal tunnel syndrome involves compression of a major nerve to your hand, producing numbness and pain in the hand. The affected hand may be more susceptible to cold temperatures.
- Repetitive action or vibration. Typing, playing piano or doing similar movements for long periods or operating vibrating tools, such as jackhammers, can lead to overuse injuries and increase your risk for Raynaud’s.
- Smoking constricts blood vessels.
- Injuries to the hands or feet such as a wrist fracture, surgery or frostbite.
- Certain medications. These can include beta blockers for high blood pressure, some migraine medications, attention-deficit/hyperactivity disorder medications and certain chemotherapy agents.
How is Raynaud’s diagnosed?
Raynaud’s is diagnosed based on your history and a physical examination. If you have primary Raynaud’s, you will typically have a normal examination and blood work. Abnormal exam and/or blood work may be associated with secondary Raynaud’s. An exam technique which involves looking at the blood vessels below the fingernails, nailfold capillaroscopy, can also be performed.
Here is a link to more information about nail fold capillaroscopy.
Who gets Raynaud’s?
Risk factors for primary Raynaud’s include:
- Gender. More women than men are affected.
- Age. Although anyone can develop primary Raynaud’s, the disease often begins between the ages of 15 and 30.
- Climate. The disorder is also more common in people who live in colder climates.
- Family history. If a first-degree relative, parent, sibling or child, has the disease, your risk of developing primary Raynaud’s appears to be increased.
Risk factors for secondary Raynaud’s include:
- Associated diseases. These include conditions such as scleroderma and lupus.
- Certain occupations. These include jobs that cause repetitive trauma, such as operating tools that vibrate.
- Exposure to certain substances. This includes smoking, taking medications which affect the blood vessels or being exposed to certain chemicals, such as vinyl chloride.
What does Raynaud’s feel like?
The symptoms of Raynaud’s can include:
- Extreme sensitivity to cold. Your body also may react to emotional stress as if it were reacting to cold.
- Skin color changes. Fingers, toes, and sometimes the ears, lips and nose, turn white due to lack of blood flow. The blood that’s left in the tissues loses its oxygen and the affected area turns blue. As fresh oxygen-rich blood returns to the area, it often turns bright red.
- Coldness, pain and numbness due to lack of oxygenated blood in the fingers. The numbness feels the same as when your hand or fingers “fall asleep”.
- Warmth, tingling and throbbing with the quick return of blood to the fingers.
- Skin ulcers and gangrene. For people with severe undiagnosed Raynaud’s and attacks that last a long time, painful, slow-healing sores may occur in the finger tips. In rare cases, a long-term lack of oxygen to the tissues can result in gangrene (when a body part loses its blood supply).
What can I do to help my Raynaud’s?
To help prevent a Raynaud’s episode:
- Bundle up outdoors. If it’s cold, put on a hat, scarf, socks and boots and mittens or gloves before you go outside. Wear a coat with snug cuffs to go around your mittens or gloves to prevent cold air from reaching your hands. You can use chemical hand or toe warmers or battery-operated heated mitts or socks. Wear earmuffs and a face mask if the tip of your nose and earlobes are sensitive to cold.
- Keep dry. Sweat that cools on the skin can trigger an attack. Wear socks, gloves, long underwear and workout clothing made from fabrics which wick moisture away from the skin. Make sure that your hair and skin are dry before you leave the gym.
- Warm your car. Run your car heater for a few minutes before driving in cold weather.
- Take precautions indoors. Wear socks. When taking food out of the refrigerator or freezer, wear gloves or oven mitts. Some people find it helpful to wear mittens and socks to bed during winter. Because air conditioning can trigger attacks, set your air conditioner to a warmer temperature. Use insulated drinking glasses.
- Avoid smoke. Smoking or inhaling secondhand smoke causes skin temperature to drop by tightening blood vessels which can lead to an attack.
- Exercise. Regular exercise can improve circulation, relieve stress and promote overall well-being. But you’ll want to avoid activities that put you at risk for numb fingers and toes or injury to the hands and feet.
- Control stress. Learning to recognize and avoid stressful situations may help control the number of attacks.
- Avoid rapidly changing temperatures. Try not to move from a hot environment to an air-conditioned room. If possible, avoid frozen-food sections of grocery stores.
- Avoid caffeine. Caffeine may trigger the symptoms of Raynaud’s. Tea, coffee, soda and chocolate may contain caffeine.
What to do during an attack:
Warm your hands, feet or other affected areas. To gently warm your fingers and toes:
- Get indoors or to a warmer area,
- Wiggle your fingers and toes,
- Place hands under armpits,
- Make wide circles (windmills) with your arms,
- Run warm, not hot, water over your fingers and toes,
- Massage your hands and feet
If stress triggers an attack, get out of the stressful situation and relax. Practice a stress-relieving technique which works for you and warm your hands or feet in water to help lessen the attack.
Alternative medicine
Lifestyle changes and supplements that encourage better blood flow might help you manage Raynaud’s. However, it’s unclear how well these measures work for Raynaud’s. More study is needed.
- Acupuncture. appears to improve blood flow, so may be helpful in relieving Raynaud’s attacks.
- Biofeedback. Using your mind to control body temperature might help decrease the severity and number of attacks you experience. Biofeedback includes guided imagery to increase the temperature of hands and feet, deep breathing, and other relaxation exercises. Your practitioner may be able to suggest a therapist who can help you learn biofeedback techniques. There are books and videos on the subject.
Talk to your doctor before taking supplements. Your doctor can warn you if there are potential drug interactions or side effects of alternative treatments.
Medical treatments
Depending on the cause of your symptoms, medications might help. Your doctor might prescribe medication to widen blood vessels and increase blood flow.
If you have severe Raynaud’s, your doctor may recommend surgery or injections.
When should I see a doctor about my Raynaud’s symptoms?
See your doctor right away if you have a history of severe Raynaud’s and develop a sore or infection in one of your affected fingers or toes.
Can a hand therapist help my Raynaud’s?
While a hand therapist won’t be able to cure your Raynaud’s, they may be able to help with an underlying condition, such as carpal tunnel syndrome. They also will have ideas and strategies for managing your symptoms.
If you’d like to book a Hand Therapy Initial Assessment click HERE.